Health Insurance Tips & Tricks
What does SEP mean and do I qualify?

RateQuote Direct,
What is this SEP acronym and does it apply to me?
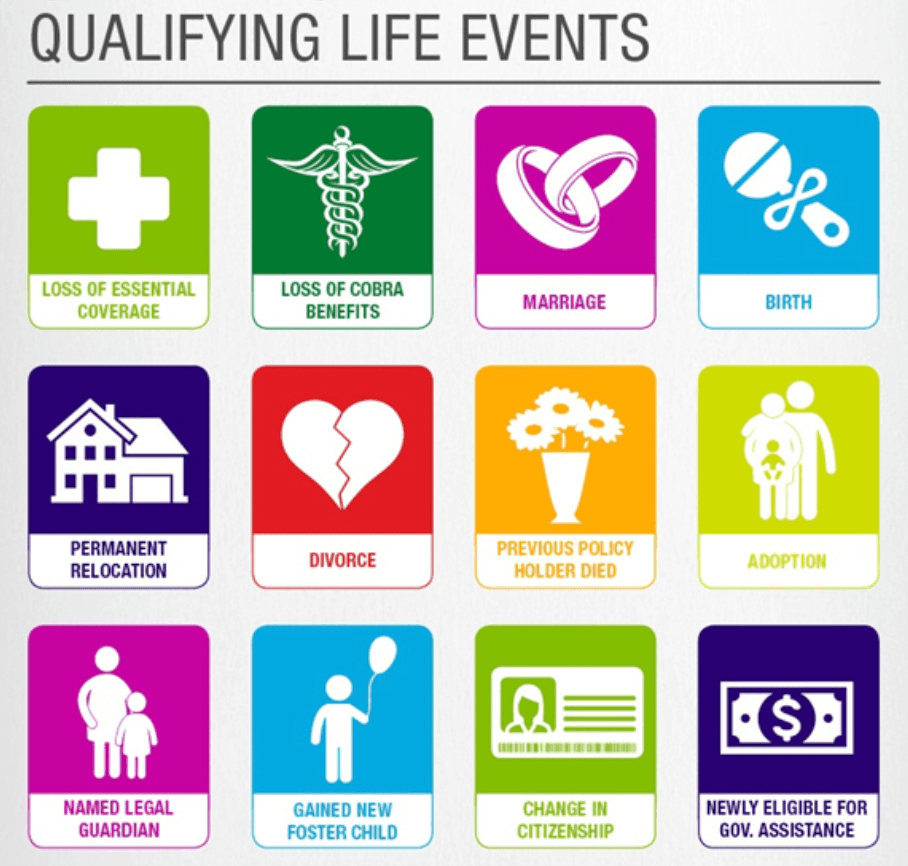
SEP stands for "Special Enrollment Period." In the context of health insurance, a Special Enrollment Period is a time outside of the regular Open Enrollment Period during which individuals and families may be eligible to enroll in or make changes to their health insurance coverage. Special Enrollment Periods are typically triggered by certain qualifying life events, such as:
1. Marriage or Divorce: Changes in marital status can often qualify individuals for a Special Enrollment Period.
2. Birth or Adoption of a Child: The addition of a new family member can be a qualifying event.
3. Loss of Other Health Coverage: If an individual loses coverage from another source, such as employer-sponsored insurance, they may be eligible for a Special Enrollment Period.
4. Change in Residence: Moving to a new area where different health plans are available may trigger a Special Enrollment Period.
5. Changes in Income: Significant changes in income or household status may make someone eligible for a Special Enrollment Period.
These are just a few examples, and the specific criteria for qualifying events may vary. During a Special Enrollment Period, individuals can enroll in a health insurance plan or make changes to their existing coverage outside of the usual Open Enrollment Period. It's important to note that proof of the qualifying event is often required when applying for coverage during a Special Enrollment Period.
It's always best to speak to a human when it comes to whether you or your family qualify under an SEP event, don't hesitate to reach out to a licensed RateQuote agent at 888-705-0122.